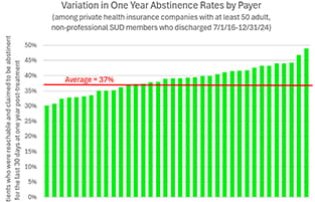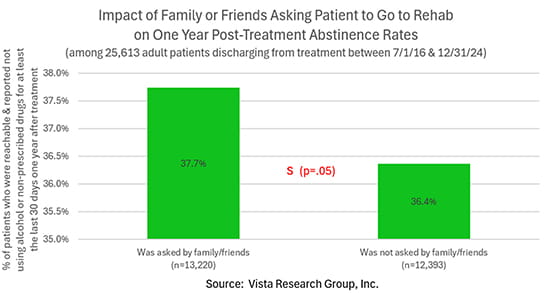
Almost half (48.5%) of patients entering addiction treatment give “Family and/or friends asked me or told me to go to treatment” as one of the primary reasons they started treatment. Interestingly, patients who were asked to go to treatment are significantly more likely to be abstinent one year post-discharge than those who didn’t report being asked:

The Blanchard Institute (TBI) offers PHP, IOP and OP levels of care in multiple locations around Charlotte, North Carolina. They believe so strongly in the importance of family support that they bake family involvement into everything they do. I talked with founder Ward Blanchard about their unique program on the latest Delivering Recovery podcast.

TBI offers three types of family programs:
Saturday Morning Family Sessions: Patients attend these weekly 3-hour sessions together with their family members or loved ones. The first 1¼ hours are educational, covering a rotating series of topics such as boundaries, communication, enabling, family roles, the disease model of addiction and family stages of recovery. After a short break, a clinician leads a process group.
Thursday Evening Resilience Meeting for Family Members Only: Every Thursday night, TBI hosts 90-minute clinician-led discussions specifically for people struggling with an addicted family member or loved one. Separate meetings are held with parents and with spouses; patients do not attend. TBI invites anyone struggling with an addicted family member to attend these meetings, regardless of whether the addicted individual is in treatment or not.
Family Weekend: Four to five times a year, TBI organizes a Family Weekend for current patients and their family members and loved ones. Held on Friday evening and all day Saturday, participants receive 12 hours of education and counseling.
TBI involves the family from the very beginning of treatment. When a patient first comes in for assessment, TBI asks them to bring their closest family members with them. While the patient is being assessed by a clinician, the family is interviewed separately. Among other things, the family is educated about the probable need for intensive PHP treatment and how important it is that their loved one stays in treatment for an extended period. TBI has found that this double-interview process dramatically increases the likelihood that the patient starts in PHP.
Nearly half of patients enter treatment because someone who loved them asked them to go. TBI didn't just acknowledge that fact; they built their entire program around it. The result is a one-year abstinence rate that puts them in the top tier of treatment centers in the country — as verified independently on Conquer Addiction.
As the mother of an addicted young adult, I know firsthand how much programs like TBI's mean to families. I hope this article and my interview with Ward Blanchard spark ideas for how you can involve families more deeply in your patients' treatment.