Every month or two, I have a discussion with one of our treatment center clients that infuriates me. After telling me that their operating costs have gone up 20% to 33% since the pandemic due to well-deserved increases in therapist compensation, they’ll add that their largest payers have increased their reimbursement rate by only 2% or 3% (or not at all) in the last five years.
The most heart-breaking conversations are with leaders of centers that I know are providing excellent treatment -- we’ve been following up with their patients for years -- who call to tell me they’re closing their doors. They just can’t provide the treatment their patients need for the money they’re being paid.
Something doesn’t add up. According to KFF, the average family's 2024 health insurance premium of $25,572 is 24% higher than it was five years ago. The payers are collecting more money from employers and consumers, but almost none of it is trickling down to addiction treatment providers.
So where is the money from these additional premiums going? No doubt some of it is being spent on expensive new treatments and medications, such as weight-loss drugs. But it’s also true that profits (earnings from operations) at the seven largest health insurance companies totaled $70.7 billion (with a “b”!) in 2023, triple what they were ten years earlier. And the CEOs of these 7 companies received $136.5 million in total compensation in 2022, an average of $19.5 million each.
Recovery Rates Vary Tremendously
By Health Insurance Company
So it’s interesting that the likelihood an individual recovers from addiction following an episode of treatment varies tremendously according to which health insurance company they have:
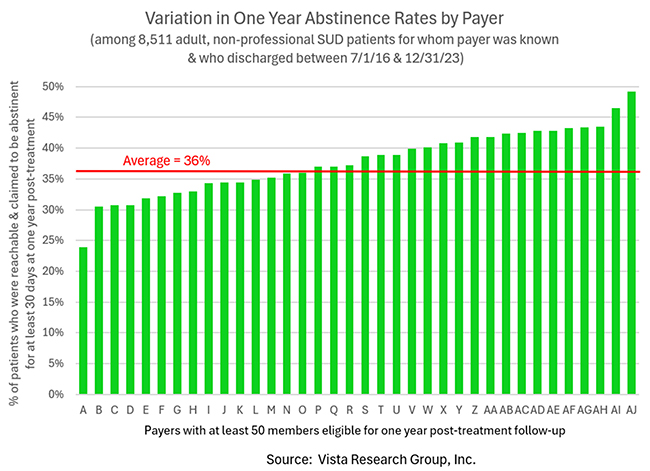
On average, 36% of individuals are reachable and report not using illicit drugs or alcohol for at least the last 30 days one year after treatment. However, 48% of the members of the insurance company with the best recovery rates are doing well one year later compared to only 24% of those with the worst health insurance. This is a shocking 2:1 difference!
It’s impossible to identify all the elements that impact a payer’s recovery rate. There are two factors, however, that are straightforward. In order for a high percentage of their members to recover:
Payers need to build a network of
highly-effective treatment centers and
they need to give their members
sufficient time in treatment to recover.
I’ve recently showcased how length of stay affects recovery rates. This chart shows how payers in the best to worst quintiles rate on both of these factors:
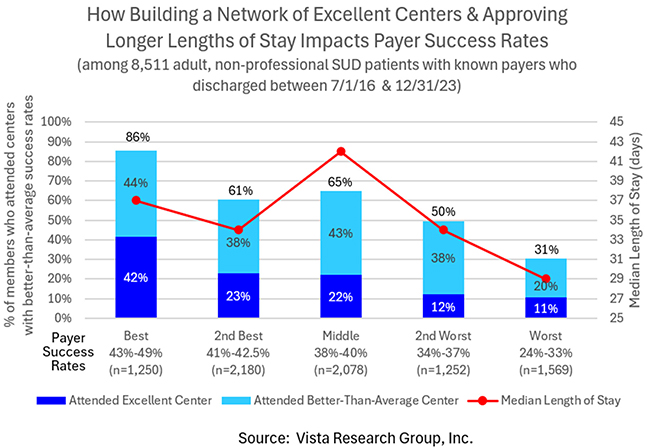
The payers with the best success rates (i.e., AD to AJ in the top chart) sent 86% of their members to treatment centers with better-than-average success rates, and patients stayed in treatment for a median length of 37 days. By comparison, only 31% of the members of the worst payers (A to H above) went to a center with better-than-average success rates, and their median length of stay was only 29 days.
These two factors are easy for a payer to control. The fact that so many payers are not bothering to manage them tells me that they aren’t prioritizing the recovery of their addicted members. Tune in next week to learn how Conquer Addiction intends to hold payers accountable for their recovery rates.
Introducing Carrum Health’s
Recovery-Focused SUD Network
To end this article on a positive note, join me in welcoming a new payer to the world of addiction treatment that IS focused on recovery. Carrum Health is building a network of addiction treatment centers with excellent recovery rates for large, self-funded employers. Qualified treatment centers are asked to define an episode of treatment, your all-inclusive bundled charge, and what you’ll do to help patients who relapse within 90 days of completing your program.
Carrum’s hyper-narrow network is filling up fast in some parts of the country. If your company has high recovery rates and you're eager to regain control over the treatment your patients receive, please join Christoph Dankert, Carrum’s Chief Network Officer, Meadow Behavioral Health's Chief Growth Officer Shannie Smith and I for the following webinar:
Partnering for Excellence: Transforming
SUD Treatment Through Value-Based Care
Wednesday, April 23rd at 2:00 p.m. EST
(1:00 p.m. CST, 12:00 noon MST; 11:00 a.m. PST)
BREAKING NEWS
Australia’s Paul King just interviewed me for two episodes of his podcast Family Support in Addiction Recovery. Please listen in below or wherever you get your podcasts:
- How Families Can Find Addiction Treatment Centers with Proven Success—Support for Substance Abuse Disorder Without Wasting Time and Money
- Why Rehab Fails Without These 3 Critical Steps for Lasting Addiction Recovery



